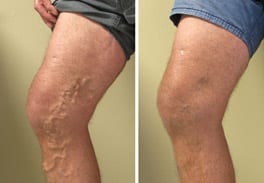
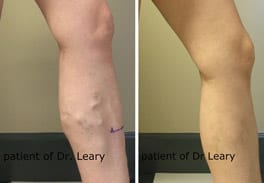
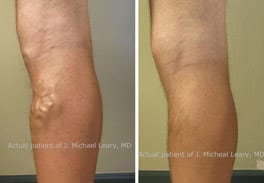
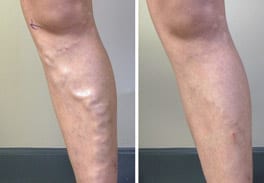
Utilizing the latest technology, California Vein Specialists is committed to providing comprehensive minimally invasive vein treatments for the full spectrum of venous disorders from painful varicose veins to cosmetic spider veins.
I have a lot of patients who come to California Vein Specialists with concerns and questions about problems with varicose veins during and after pregnancy. Varicose veins usually make their first appearance during pregnancy. Population studies have shown that only 12% of women who have varicose veins have never been pregnant!
Certifications
- American Board of Venous & Lymphatic Medicine
- American Board of Emergency Medicine
Professional Memberships and Accreditations
- Member, American College of Phlebology
- Diplomate, American Board of Venous & Lymphatic Medicine
- Member, American Venous Forum
- Member, American Society of Laser Medicine and Surgery
- Member, American Board of Emergency Medicine
- Fellow, American Board of Emergency Medicine
There are many reasons pregnancy has an adverse effect on leg health. Total body fluid increases 40 to 50 percent and there is significant sodium retention. This may cause edema (swelling) in the lower legs and ankles.
Hormonal effects are responsible for the venous dilation that occurs during pregnancy. High levels of the hormone progesterone weaken vein walls. Estrogen causes veins to dilate. Relaxin also causes the veins to dilate.
The enlarging uterus in pregnancy causes the large femoral veins to become obstructed. This causes an increase in the venous pressures of the lower legs.
 Pregnancy is also a significant risk for superficial and deep venous blood clots. Many coagulation factors are activated during pregnancy. This hypercoagulable state may increase the risk of a blood clot, especially post partum. This hypercoagulable state is caused by the increased blood volume, the enlarged uterus which obstructs venous return, and elevated hormonal levels that increase vein distensibility.
Pregnancy is also a significant risk for superficial and deep venous blood clots. Many coagulation factors are activated during pregnancy. This hypercoagulable state may increase the risk of a blood clot, especially post partum. This hypercoagulable state is caused by the increased blood volume, the enlarged uterus which obstructs venous return, and elevated hormonal levels that increase vein distensibility.
 Graded compression hose worn during pregnancy can reduce the pressure in your legs and the swelling. It is a good idea to wear them when you are going to be standing for long periods or sitting for long periods. Elevating your legs as much as possible is also helpful. Graded compression hose also are proven to reduce the risk of blood clots so it should be worn before, during and immediately after delivery. Early ambulation after delivery is also important to reduce your risk. If you have a history of blood clots or someone in your family has a history, you should have a thrombophilic risk work up. This is a series of blood test to see if there are factors in your blood that make you more prone to clots. If you are found to be at risk there are steps that can be taken to reduce your risk. Exercise is important. Any exercise that develops a good calf muscle is important. Remember the calf muscle is the main pump that pumps blood through the veins. Walking, hiking, swimming and biking are all great for leg health during pregnancy. A lot of my patients are avid runners, I think it is important to wear compression hose if you plan to continue running during your pregnancy. This will help reduce the pressure in your legs and may help protect the valves. Try to sleep on your left side. The uterus compresses the pelvic veins and vena cava more when lying on your right side. This in turn increases the venous pressure in your legs leading to more strain on the valves.
Graded compression hose worn during pregnancy can reduce the pressure in your legs and the swelling. It is a good idea to wear them when you are going to be standing for long periods or sitting for long periods. Elevating your legs as much as possible is also helpful. Graded compression hose also are proven to reduce the risk of blood clots so it should be worn before, during and immediately after delivery. Early ambulation after delivery is also important to reduce your risk. If you have a history of blood clots or someone in your family has a history, you should have a thrombophilic risk work up. This is a series of blood test to see if there are factors in your blood that make you more prone to clots. If you are found to be at risk there are steps that can be taken to reduce your risk. Exercise is important. Any exercise that develops a good calf muscle is important. Remember the calf muscle is the main pump that pumps blood through the veins. Walking, hiking, swimming and biking are all great for leg health during pregnancy. A lot of my patients are avid runners, I think it is important to wear compression hose if you plan to continue running during your pregnancy. This will help reduce the pressure in your legs and may help protect the valves. Try to sleep on your left side. The uterus compresses the pelvic veins and vena cava more when lying on your right side. This in turn increases the venous pressure in your legs leading to more strain on the valves.
Leg treatments during pregnancy
In general leg vein treatments should be postponed until after the pregnancy and after you have completed breast feeding. Hormonal changes may remain four to six months postpartum. Many times the enlarged veins of pregnancy may become normal again after the hormonal influence has been reduced. Sclerotherapy solutions are very safe, but should not be administered during pregnancy or lactation.
Other vein problems after pregnancy
Pelvic obstruction may be a cause of vulvar varicosities. This can occur in the third trimester. Vulvar varicosities that remain after pregnancy may become quite painful, usually during menses or even intercourse. They are easily treated with sclerotherapy, usually with complete resolution.
How to prevent Varicose Veins during Pregnancy
You may or may not be able to prevent varicose veins during pregnancy. Fortunately you can take steps to minimize the severity of varicose veins and treat the veins you do have during pregnancy. Here are some simple steps for treating and minimizing varicose veins during pregnancy:
It is good to exercise regularly to help promote your circulation and decrease the risk of blood pooling in your veins. Even a short walk around the block can help keep your cardiovascular system functioning well.
Elevate your feet often to increase blood flow. This is important whether you are at work at your desk or lying down at night. When your legs become fatigued and sore, try to sit with your feet propped up on a table or chair. Also try to sleep with your feet elevated on a pillow. Sleep on your left side. The largest vein in your body is the vena cava and carries the largest amount of blood through your body. Because it is located on the right side of your body, lying on your left side will decrease added pressure on the vein.
Avoid standing or sitting still for long periods of time. Take frequent breaks to stretch while at your desk and shift your weight while standing. This can help decrease the amount of pressure on your legs and help keep your circulation moving. Wiggle your toes regularly and flex your muscles to also promote better circulation in your legs.
Buy some pregnancy support hose that provide graduated compression. This will not only help reduce bulging but will also help reduce any swelling you experience in your extremities during pregnancy. These stockings unlike normal pantyhose are quite thick and help maintain blood circulation. They can also help prevent blood from pooling in your legs if you put them on first thing in the morning. Put them on before you stand up out of bed in the morning. By putting them on before standing you will prevent blood from pooling in your lower legs.
Try to rest frequently. Because your growing uterus is putting added pressure on the veins in your lower body, blood flow can become strained causing larger and swollen veins in your legs, vulva and rectum. Increasing hormones also relax the walls of your veins as well as the ligaments and joints in your body. The less you exert your body, the less pressure you will put on your veins.
*Providing you with accurate medical information is one of our priorities. To ensure this, Dr. Leary reviews all the information posted on our website. Please get in touch with us today if you would like more information about any of the conditions we treat and the procedures we offer.